
A transfusion reaction report was filed no clerical discrepancies were found.Ī visual hemolysis check comparing plasma from pre- and post-transfusion specimens taken 15 min after the initiation of the transfusion showed mild hemolysis - change of grade from 1 to 2 on hemolysis scale with grade range 1 to 8 (Haemonetics, Braintree, MA, USA). 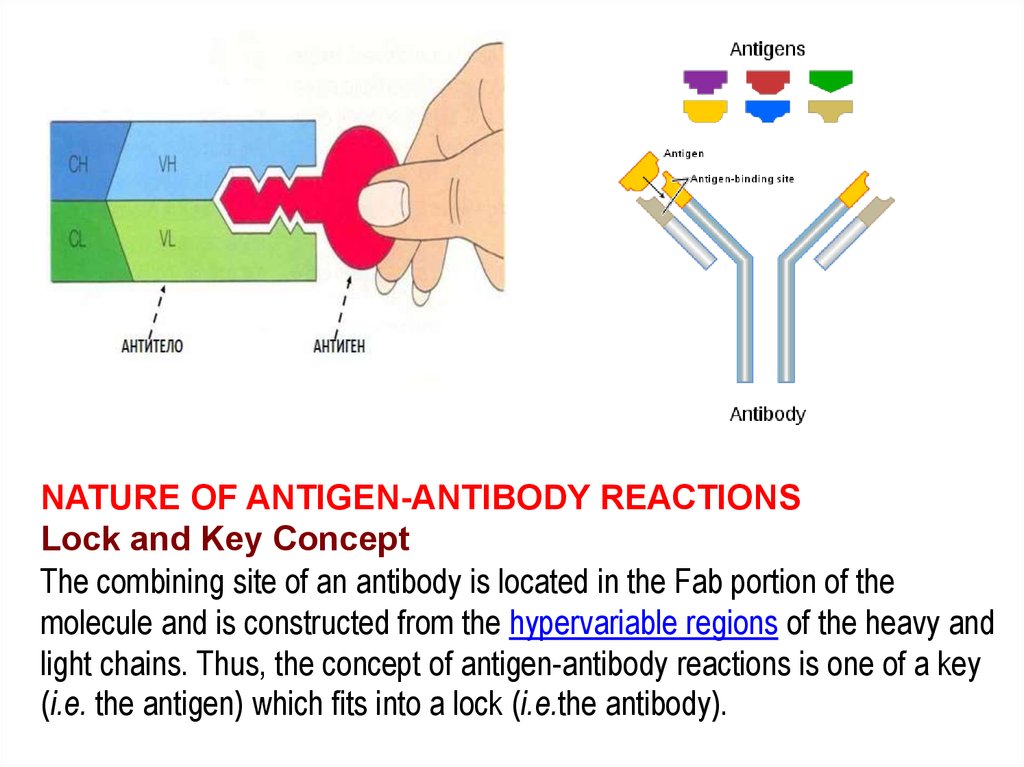
Patient was febrile at initiation of transfusion, and no significant change in temperature occurred during transfusion. Vital signs showed significant elevation of blood pressure all other vital signs were stable (table (table1). At 87 min into the transfusion (approximately 175 ml given), the patient developed chills and rigors and transfusion was discontinued. On the following day, another unit of RBCs was ordered (electronic crossmatch) and transfused. 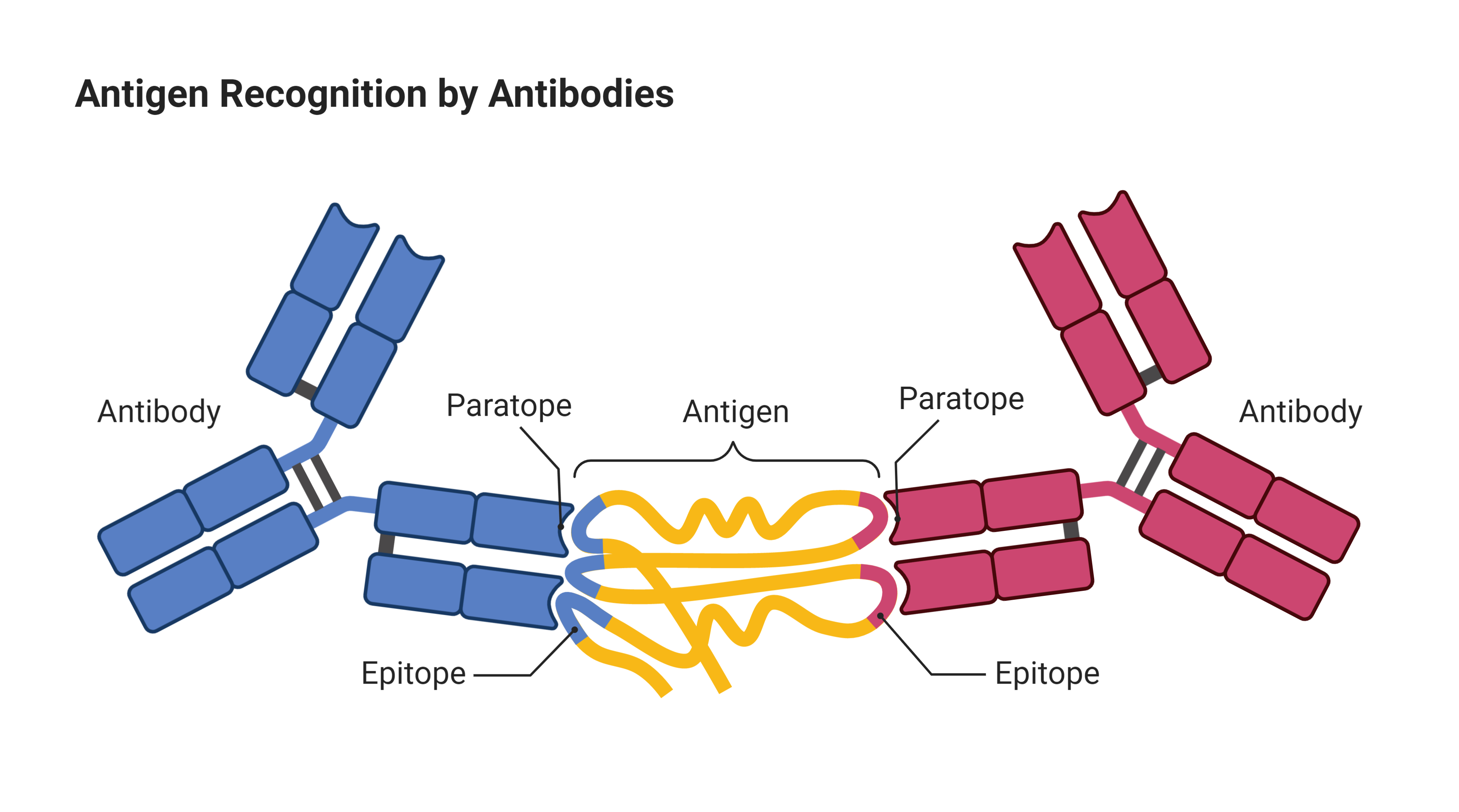
On date of admission, the patient received two RBC units and two platelet units without incident all cellular components were pre-storage leukocyte-reduced and irradiated. Electronic crossmatch was used for RBC compatibility confirmation. Patient pre-transfusion testing showed blood group A, RhD-positive and negative antibody detection test (Capture-R solid phase Immucor, Norcross, GA, USA). Fluorescent in situ hybridization (FISH) confirmed t(15 17)(q24 q21) translocation. Flow cytometric analysis demonstrated CD117-positive myeloid blasts representing 88.9% of the white cells with features consistent with APML: increased CD33, variably decreased CD34, increased CD117, and low to absent HLA-DR. Peripheral blood smear morphology revealed abnormal promyelocytes and myeloid precursors, concerning for acute promyelocytic leukemia (APML). He was given fluids, started on cefepime and vancomycin, and transferred to a tertiary medical center. In the ED the patient was found to be febrile to 39.0 ☌, tachycardic to 118 bpm, mildly hypertensive to 157/78 mm Hg, and pancytopenic with white blood cell count of 3.1 × 10 3/μl, platelet count of 11 × 10 3/μl, and hematocrit of 17%. He was given antibiotics and sent home but was later called and advised to go to the emergency department (ED) for evaluation of pancytopenia. The patient presented to urgent care clinic for a non-painful skin infection over his left nipple. Ī previously healthy 36-year-old man developed weakness, fatigue, easy bruising, and oral mucosal bleeding. Mild cases of delayed HTR may be more frequent. These reports implicate both IgG and IgM classes of anti-P1 as a cause of severe HTR. However, rare cases of severe acute and severe delayed hemolytic transfusion reactions (HTRs) caused by anti-P1 antibodies reactive at 37 ☌ have been reported. Anti-P1 is typically a clinically insignificant IgM antibody that does not react at temperatures >25 ☌. Anti-P1 antibody is frequently present in P 2 individuals (∼67%) and most often naturally occurring. The P 1 phenotype is present in 79% of Caucasians, 94% of African Americans, and 20% of Cambodians and Vietnamese. P 2 individuals are missing the P1 antigen on the RBCs' surface but still synthesize P k and P antigens through the globoside synthesis pathway. Paragloboside (lacto-N-neotetraosyl ceramide) is converted to P1 by the addition of an alpha-galactosyl residue. P antigens, including P1 and P k antigens in the P1PK system and P antigen in the GLOB system, are synthesized by sequential addition of monosaccharides by glycosyltransferase enzymes to precursor glycosphingolipids.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
